How serious are we about asepsis for rodent surgery?

As part of the NC3Rs year of laboratory rodent welfare, our latest blog is from Professor Paul Flecknell, Newcastle University on the issue of aseptic surgery.
Paul is a world renowned laboratory animal veterinarian who specialises in anaesthesia and analgesia.
A rumour circulated recently amongst UK lab animal veterinarians that the Home Office Inspectorate (the UK regulator for animal procedures) intended to ban the use of hot bead sterilisers. For those of you unfamiliar with this device, it is designed to sterilise the tips of surgical instruments by rapidly heating them to over 200oC. This is useful when undertaking surgery on several rodents in succession, so called ‘batch surgery’, to allow decontamination of the instrument tips between successive animals. However, since it is only the instrument tips that are sterilised there are concerns that this compromises measures taken to keep to an absolute minimum the risk of infection of the surgical wound. My first reaction to this rumour was “good, but what are they suggesting as an alternative, and will they also make mandatory some of the more important recommendations in their last guidance note?”
The obvious alternative to using a hot bead steriliser is to have a separate set of sterilised instruments for each animal – and of course a clean sterile drape. The surgeon would also need to change their gloves and perhaps their surgical gown. When operating on twenty or more animals in a single session, this would introduce considerable resourcing issues and, not surprisingly, those conducting the procedure might ask for evidence of the benefit of this recommendation.
And here’s the problem – we lack robust scientific data, obtained in rodents, to support these measures. We do, however, have a great deal of evidence in other species that aseptic technique – reducing to a minimum any contamination of the surgical site with micro-organisms – is essential to prevent post-operative wound infections. We know that similar numbers of bacteria are needed to establish wound infections in rodents and other species (including people) and some procedures such as implanting catheters in blood vessels have an earlier failure rate if good asepsis is not observed.
However, in contrast to other species, rodents rarely develop obvious signs of wound infection and the signs associated with infection are often subtle. This led to suggestions in the 1960s and 70s that aseptic technique was unnecessary in rodents, and this was reflected in very poor standards. Current legislation is vague on this issue, but the learning outcomes for the relevant EU (and UK) training module are clear, stating at several points the need for an understanding of asepsis. Guidance from regulators tends to insist on asepsis for surgery with larger species, but often relaxes those standards for rodents.
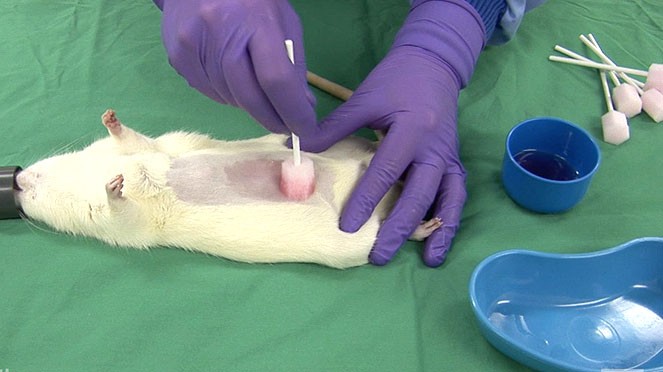
So what should we be doing, to obtain reliable, reproducible results, without the confounding effects of wound infections? Clearly, in addition to improving scientific outcomes, there are significant welfare benefits to avoiding these complications. We tried to set out what appeared an appropriate compromise in the online resource ‘Procedures with care’, trying to combine good practice with practical considerations. Essentially, our recommendations were to start with sterile instruments, wear sterile gloves, use a sterile drape, shave and disinfect the surgical site, as recommended in Home Office guidance. The procedure should then be carried out in a way that minimised contamination of the operator and the instruments. The instrument tips could be cleaned and sterilised in a hot bead steriliser, and the drape replaced for the next animal. If only the instrument tips were in contact with the surgical site, then the risk of wound infection should be low. If obvious contamination of the instruments or the surgeon’s hands occurred, then a fresh set of instruments should be available and the surgeon should re-glove.
Achieving this compromise approach is almost impossible without the use of an assistant. Undertaking surgery requires numerous ‘support’ tasks, not least preparing successive animals for surgery. This requires handling of animals and the cage, shaving them, cleaning the surgical site and also handling items and apparatus needed for anaesthesia. Even relatively brief anaesthetics for short procedures can result in problems, and animals need to be observed throughout to allow these to be dealt with promptly. It’s hard to do this while concentrating on performing surgery competently. It is possible to perform all the other required actions, but the surgeon then needs to re-scrub, re-gown, and re-glove. If adjustments are needed to the anaesthetic machine, or to re-position the animal, or open a fresh pack of sutures, then such tasks are much more time consuming and difficult without compromising asepsis.
Despite all these issues, we are repeatedly asked on our EU22/Pil C training courses “What do I do if I don’t have an assistant?” The obvious answer is “hire one” or more realistically, recruit the help of someone else in your research group. In many facilities, technical staff can be hired on an hourly rate to assist – a cost that can easily be incorporated into a grant application. If this source of assistance is not available, then small research groups can surely co-operate and help each other? We’ve used this approach for complex behavior studies, and repaid the loan of a PhD student or post-doc’s time with similar help to our colleagues.
One study that we need to repeat and document more carefully, was an exercise we conducted some years ago during a training course. We set up two operating tables and, using post-mortem material, carried out five laparotomies in sequence – one group operated solo, the other had an assistant. Both groups had to adopt the standards of asepsis outlined above. The result – the group with an assistant completed the surgery in half the time.
So to conclude, why not stop worrying about whether to use hot bead sterilisers or not, and focus on making some of these other processes mandatory? Once we have a better evidence base, we can consider whether current recommended standards of asepsis need revision, but in the meantime, let’s make sure these recommendations are properly implemented. It makes no sense to teach new research workers the importance of asepsis, but then tell them they don’t need to apply their training to their own work.
